Tag: Metabolic Health
-

Diet Doctor launches Hava.co. Is a satiety score a good thing?
Diet Doctor, long known for it’s advocacy and education surrounding the Keto Diet and living a low carb lifestyle, has launched a new company named Hava. Hava seeks to fill a void for people who feel they can’t sustain a life-long commitment to the Keto Diet by focusing on satiety. This innovative approach and our…
-

Mitochondria dysfunction may be the common denominator between metabolic & mental health problems
Dr. Christopher M. Palmer, a Harvard researcher and psychiatrist, wrote a book called “Brain Energy: A Revolutionary Breakthrough in Understanding Mental Health and Improving Treatment for Anxiety, Depression, OCD, PTSD, and More. Yes, I know, that subtitle is a mouthful. In Brain Energy, Dr. Palmer connects mitochondria dysfunction to mental health issues like Parkinson’s, Alzheimer’s,…
-
Study shows positive effects for bipolar disorder while on the Ketogenic Diet
The study out of Poland is about how the ketogenic diet can help people with bipolar disorder. Sometimes medications do not work well for people with bi polar disorder, so they need other ways to treat their condition. The study reports the case of a man who had bipolar disorder and tried a ketogenic diet.…
-

The Best Ways to Get Your Family to Eat Healthy
By: Sheila Johnson of wellshelia.net When your family has a schedule that’s packed with activities, it can be easy to reach for the quickest option to feed them each day. However, opting for fast food and processed snacks can take a toll on your family’s long-term health, and you all may end up with less energy…
-

Improve Your Overall Wellness With These Lifestyle Changes
By: Sheila Johnson of wellshelia.net Life can be stressful, and it’s easy to get bogged down in the daily grind. Between work, family commitments, and trying to juggle a social life on top of it all, it can be difficult to find time for yourself. If you’ve been struggling with your physical or mental health lately,…
-
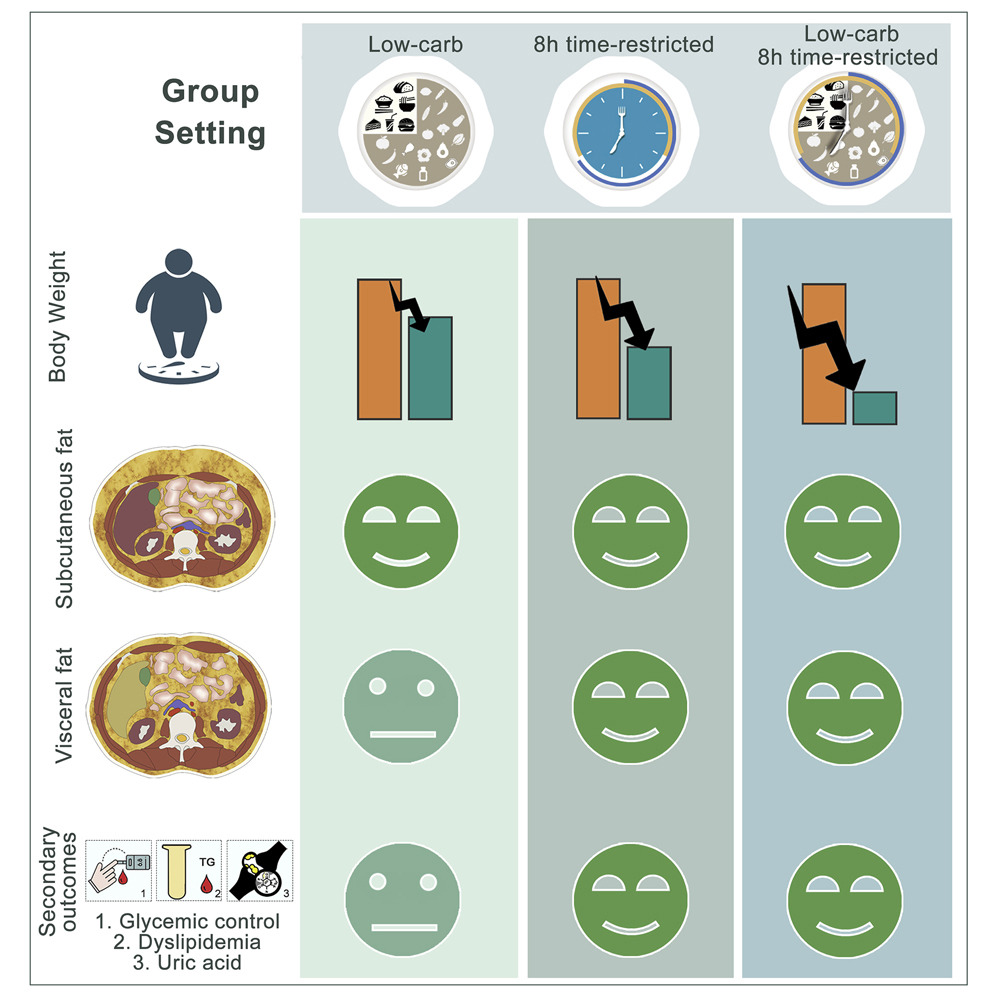
Study: Time restricted eating is an effective intervention for metabolic syndrome
Reducing visceral fat is extremely important. That’s the fat you can’t see. It’s the fat that builds up in your organs and will kill you over time. There is something called “skinny-fat” which describes someone who looks fit or healthy from the outside but has fat surrounding their internal organs. There are so many acronyms…
